Healthcare is evolving quickly, driven by a growing recognition that health outcomes depend on more than episodic encounters or isolated data points. Today, the most effective systems are connected ones, where clinicians, families, administrators, researchers, and payers share timely information and collaborate seamlessly.
This shift toward connected care is not simply a technological upgrade; it’s a fundamental redesign of how healthcare is delivered, experienced, and measured. It enables a more complete understanding of individuals and populations while supporting models of care that focus on prevention, coordination, and shared accountability.
Defining Connected Care
The connected care delivery model uses technology to link patients, providers, and data across all care settings—enabling continuous monitoring, coordinated decision-making, and proactive intervention.
Connected care is often associated with digital tools or remote technologies, but its core is much broader. It brings together:
- Continuous, contextual data rather than intermittent snapshots
- Communication pathways that link all stakeholders
- Integrated systems that reduce fragmentation
- Collaborative workflows across care settings
- A shared understanding of patient needs, risk, and progress
This ecosystem view shifts healthcare from reactive problem-solving to proactive, coordinated care.
Why Connected Care Matters More Than Ever
Three converging pressures are making connected care critical for value-based care models:
1. Healthcare is too complex to operate in silos
Care teams today manage higher patient acuity, more chronic conditions, and more diverse care settings. Without shared data and communication channels, gaps form: gaps that create barriers to quality, safety, and efficiency. Connected care fills these gaps with continuity.
Consider a patient discharged from a hospital on Friday afternoon with new cardiac medication. By Monday morning at the skilled nursing facility, their heart rate has gradually increased from 76 to 98 beats per minute—a 40% increase over 72 hours—but because the hospital’s discharge summary didn’t include their baseline vitals and the SNF uses manual spot checks every 4 hours, no one recognizes this as a deviation. By Wednesday, the patient is back in the ER.
2. Patients move – their data should too
People transition between hospitals, clinics, rehabilitation centers, and home environments. Connected care ensures that their information, context, and risk factors move with them.
A patient recovering from pneumonia is discharged from the hospital on Friday with home health services. The hospital documented a resting respiratory rate of 12 breaths per minute at discharge. By the following Wednesday, the home health nurse measures 22 breaths per minute during her visit—but without access to the baseline from five days earlier, this looks “within normal limits” rather than an 83% increase signaling incomplete recovery or early relapse.
3. Preventive strategies need context and coordination
Prevention depends on shared insight, aligned plans, timely response, and awareness of individual trends. Connected care enables that foundation.
A 78-year-old resident with a history of depression was recently changed to a new antidepressant to treat his insomnia. After two days on the medication, he shows subtle overnight respiratory changes on Tuesday and Wednesday—slight increases in respiratory rate and shifts in breathing patterns that are too small to trigger individual alerts but concerning when viewed as a two-day trend. The night nurse, the attending physician, and the care plan coordinator all need to see the same pattern to decide whether to adjust the dosage, discontinue the medication, or monitor more closely. Without a shared view, they each see only fragments.
These challenges intensify as staff shortages collide with the expected increase in the elderly population.

Sources: HRSA Health Workforce, Mercer, PRB
Early Detection’s Role in Connected Care
Early detection is not the “centerpiece” of connected care, but it plays an important supporting role. When ecosystems are connected:
- Subtle changes are recognized more quickly
- Teams can intervene sooner
- Families stay informed
- Care plans adjust before issues escalate
- Transitions between settings become smoother

Clinical data from five skilled nursing facilities show that continuous monitoring can provide an average 5-day window before hospitalization becomes necessary—time that can transform crisis response into planned intervention.
The Impact of Connected Care Across Stakeholders
Clinicians: Better data and decisions, instead of disconnected data points
Connected care gives physicians, nurses, and allied health professionals the context they need to make confident decisions. By seeing trends over time and across settings, clinicians can understand baselines, identify deviations more quickly, coordinate care with other teams, and reduce delays caused by missing information.
Families: Clearer communication and shared understanding
Families often serve as advocates and caregivers. With access to more transparent, continuous information (with consent), they gain greater involvement in decisions, more insight into progress or decline, and a stronger partnership with care teams.
Administrators: Operational awareness across the continuum
From staffing to bed allocation to performance metrics, administrators rely on accurate, timely information. Connected care supports smoother care transitions, better resource planning, reduced variability across departments, and enhanced quality and safety outcomes.
Payers: A more predictable and preventive risk landscape
When care is connected, payers can better understand member risk trajectories, where preventive interventions are needed, how care pathways influence outcomes, and which populations benefit from targeted support.
Researchers: Meaningful insight from real-world patterns
Continuous, connected data creates research opportunities that reflect true physiological trends, long-term behaviors, real-world care patterns, and population-level insights.
How Value-Based Care Fits into the Connected Care Ecosystem
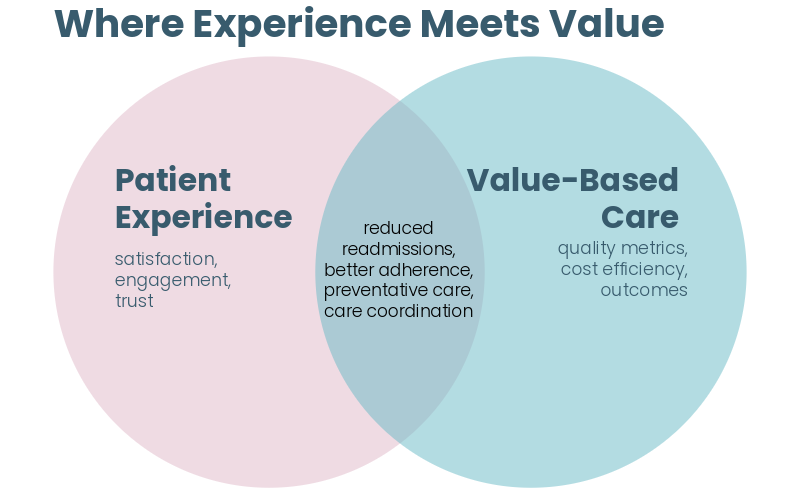
Value-based care and connected care reinforce each other naturally. Where value-based care emphasizes outcomes, prevention, coordination, experience, and efficiency, connected care provides the infrastructure that makes these goals achievable.
Rather than being a strategy on its own, connected care enables value-based care by supporting greater transparency, improving continuity between providers, reducing preventable deterioration, lowering operational friction, and strengthening patient and family engagement.
As healthcare leadership increasingly focuses on improving the patient experience, the interconnection with value-based care is undeniable.
The Technology Behind Connected Care
Technology does not define connected care; it simply enables it. Two capabilities play an important role:
AI-Enabled Clinical Insights
AI helps transform raw data streams into meaningful insights such as trends, variations, patterns, and population-level comparisons. These insights allow teams to act sooner and with greater clarity.
System Integration and Interoperability
For connected care to function, data must flow across departments, across care settings, into workflows, into records, and into communication channels. Integration is what makes connected care seamless instead of burdensome.
A Future Rooted in Collaboration, Continuity, and Shared Purpose
Connected care is not a feature. It is a philosophy grounded in the belief that healthcare works best when every participant is informed, aligned, and continuously supported by insight.
As healthcare continues its shift toward value-based models, connected ecosystems will separate sustainable organizations from those struggling with fragmentation and reactive care. The infrastructure is available. The evidence is compelling. What remains is leadership commitment to coordination over silos, prevention over intervention, and collaboration over isolation.
Most importantly, connected care creates a healthcare environment where every decision is made with better context, better coordination, and better clarity. That difference defines the future of sustainable healthcare delivery.
Ready to see how continuous, contactless monitoring supports your connected care strategy?
Neteera’s sensor technology provides the early detection layer that connected care requires—delivering an average 5-day advance warning before hospitalization with 89% accuracy for cardiac and respiratory events. Integration with existing workflows enables care teams to act on changes before they become crises. See a demo.


