Choosing a patient monitoring system is one of those decisions that ripples through your entire organization.
Get it right, and you’ll have a tool that supports early detection, enables smoother workflows, and helps clinical teams focus on patients instead of wrestling with technology. Get it wrong, and you’re stuck with expensive equipment that nobody uses, data that doesn’t flow where it needs to go, and frustrated staff working around the system instead of with it.
The global market for patient monitoring solutions is expected to reach nearly $80 billion by 2029, an 11.96% increase since 2023. What’s driving this forecasted growth? Healthcare facilities are seeing real results from patient monitoring—fewer transfers, earlier detection of deterioration, and better resource use. If you’re not evaluating solutions now, you likely will in the near future.
This guide helps you ask the right questions, see beyond the sales pitch, and determine what really matters for your facility when choosing your patient monitoring solution.
What You Need in a Patient Monitoring Solution (Not What Vendors Want to Sell You)
Monitoring Detection Accuracy
Start with this question: Does the system accurately detect changes in patient condition in time for clinicians to intervene before conditions worsen?
Lab-tested numbers aren’t road-tested. Ask about real-world performance instead. Vendors should be able to provide real-world performance data. Solutions are available that achieve over 75% accuracy in clinical settings. Pair that detection accuracy with early warning capabilities appropriate to your setting.
For acute care:
Look for hospital monitoring technology that can identify changes in patient condition days in advance. Studies demonstrate that 80% of ICU transfers occur within the first 48 hours of admission—the critical window when monitoring is most important. Research shows that continuous monitoring can identify risk an average of 18 hours or more before clinical intervention is necessary, giving your team time to prevent deterioration, rather than react to a crisis.
For post-acute care:
In post-acute care settings like SNFs, rehab facilities, and home health, prioritize continuous monitoring solutions that track gradual baseline changes over multiple days. Patients in these settings deteriorate more slowly than acute care patients. Look for systems that establish individual baselines and detect subtle changes over 3-5 days, enabling early intervention before hospitalization becomes necessary.
Monitoring Technology Integration That Actually Works
Most electronic health records, medical devices, and IT systems don’t talk to each other. Your clinicians end up without a complete view of what’s happening with their patients.
Your new vital signs monitoring system needs to fit into your existing setup without a heavy IT lift. Not through workarounds or manual data entry—through actual, working integrations.
Ask the vendor to demonstrate how data flows between their system and your EHR. Don’t accept vague promises.
This example illustrates the data flow from capture to the user for the Neteera monitoring system:
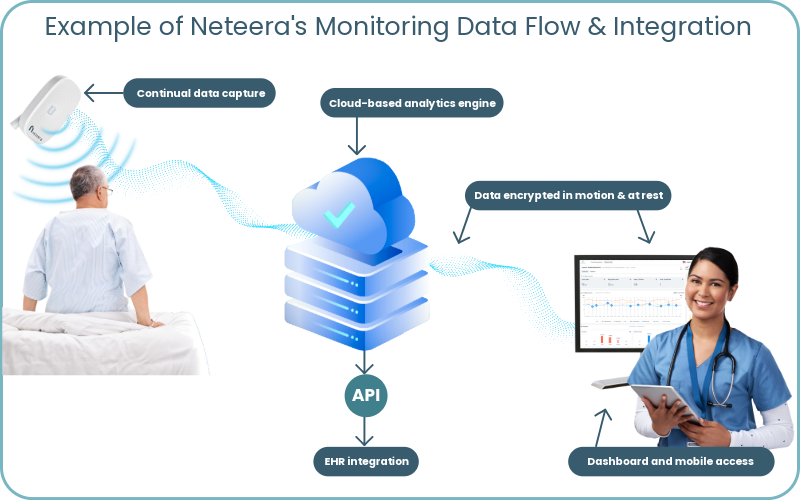
When data flows seamlessly, your team can focus on patients instead of playing data detective across multiple systems.
Monitoring Settings That Adapt to Your Reality
Every facility is different. Emergency department (ED) alert parameters won’t be the same as post-acute care. Each patient population has unique needs.
The patient monitoring system should let you adjust sensitivity settings based on your actual patient populations and clinical protocols. One-size-fits-all configurations don’t work in real healthcare environments.
Non-Negotiables for Patient Monitoring
Technology Your Staff Will Actually Use
Clinical personnel prioritize user-friendliness and clear visualizations. This makes sense—if your nurses and clinicians can’t quickly figure out the system, they won’t use it.
When evaluating usability, be sure to include mobile accessibility. Your staff need to check alerts and patient data from anywhere in the facility, not just at fixed workstations.
Quality reporting and analytics should be built in, not bolted on. You’re investing in this system to improve outcomes.
Support That Doesn’t Disappear After Installation
The vendor’s job doesn’t end when the system goes live. You need reliable technical support and training during implementation and as your needs evolve.
Does the vendor offer staff training before and after deployment? New staff need to be onboarded, and existing staff may need refresher training.
What support channels are available? Understand response times, escalation procedures, and how quickly you can get help when issues arise.
Ask about continued software development and improvements. Technology moves fast. Your monitoring system shouldn’t feel outdated in two years.
Cybersecurity and Compliance Are Patient Monitoring Essentials
Regulatory compliance isn’t negotiable. In the United States, FDA clearance is required for vendors to legally market and sell patient monitoring devices. Healthcare facilities must ensure they’re purchasing FDA-cleared solutions—using non-cleared devices creates liability exposure, potential regulatory violations, and complications with Medicare/Medicaid reimbursement.
In Europe, devices must comply with Medical Device Regulation (MDR) requirements and display CE marking with the four-digit notified body number. Both regions require data protection compliance: HIPAA in the United States and GDPR in Europe.
Ask about security certifications, specifically SOC 2 and ISO 27001, and independent cybersecurity audits. SOC 2 demonstrates that vendors follow strict data security practices, while ISO 27001 shows they maintain comprehensive information security management systems.
What happens to the patient data collected? Is it encrypted both at rest and in transit? Who owns the data, and how easily can it be accessed or exported for reporting purposes?
Don’t assume compliance. Ask for documentation.
Common Monitoring Mistakes That Cost You Later
Shopping on Price Alone
Hospitals spend nearly $25 billion annually on supply chain inefficiencies due to poor vendor management. The cheapest option usually becomes the most expensive.
When you factor in poor detection rates, integration nightmares, and staff turnover linked to poor tools, a “bargain” system can cost you multiples of what you saved.
Calculate the total cost of ownership, not just the purchase price. Include hardware, software, implementation, training, ongoing support, and hidden integration costs. That’s your real number.
Skipping the Due Diligence
Don’t just take the vendor’s word for it. Ask the vendor to provide you with contact information for other providers using the system.
Ask these contacts:
- What surprised you during implementation?
- How’s the ongoing support?
- Have your costs been what you expected?
- Would you buy it again?
Doing your due diligence should also include the vendor’s financial stability. A monitoring system is a 5– to 10-year investment. You need that vendor to be around to support it.
Underestimating Change Management Needed for Patient Monitoring
Technology alone doesn’t improve outcomes. People using the technology improve outcomes.
Budget time and resources for staff training. Plan for workflow adjustments. Identify champions who can help their colleagues adapt. The best monitoring system in the world fails if your team doesn’t embrace it.
Making Assumptions About Support and Training
The system goes live. Then what? Your needs will evolve, and vendor support determines whether your investment succeeds or the technology gets shelved.
Patient populations shift. Regulations change. Staff come and go. Vendors shouldn’t treat support and training as an afterthought. You need a vendor that supports the future after deployment.
Questions That Get to the Truth
Ask these questions. Listen carefully to how vendors answer—and what they avoid answering.

Easily Compare Patient Monitoring Vendors Side by Side
Use this interactive scorecard to compare vendors against essential criteria when choosing a patient monitoring system.
About Clinical Performance
“What evidence supports your solution’s impact on outcomes?”
You want studies, not marketing materials. Many monitoring systems get stuck in pilot phases and never scale to full clinical deployment. Verify this system has moved beyond pilots to proven, sustained implementation.
“What’s your detection accuracy rate in real-world implementations?”
Lab results don’t always translate to busy care environments. Ask for real-world data from facilities like yours—not cherry-picked, best-case scenarios.
“Which conditions or patient populations are best suited for this solution?”
No monitoring system is perfect for every use case. The vendor should be honest about where their system excels and where it doesn’t. If they claim it’s perfect for everything, they’re overselling.
“How do you integrate with our existing EHR system?”
Get specific. Don’t accept vague promises. Ask which version of your EHR they’ve integrated with, how long it typically takes, and who owns the integration work.
“What workflows are automated vs. manual?”
The more manual steps required, the more likely workflows are to break down during busy shifts. Map this out before you commit.
“Can alert parameters be customized?”
Different settings have different needs. Make sure you can configure accordingly.
About User Experience
“How easy is it for clinicians to use?”
Both patients and healthcare providers expect intuitive, accessible systems—that’s what drives adoption.
“How do you minimize false positives and alert fatigue?”
Some patient monitoring systems trigger frequent false alarms. This desensitizes providers, potentially leading to slower response times or missed critical alerts. Ask how they’ve addressed this specific problem.
If it’s a patient-operated system, add these questions:
“How easy is it for patients to use?”
Complex systems lead to poor compliance. Poor compliance leads to missing data and failed monitoring. Simple wins here.
“What features drive patient adherence and engagement?”
Look for simplicity, comfort, and feedback mechanisms that keep patients engaged with their own monitoring.
“How do you support patients with limited digital access or literacy?”
Not every patient has a smartphone or strong tech skills. Your monitoring solution needs to accommodate everyone in your patient population.
About Data and Analytics
“How is data captured, transmitted, and displayed?”
Real-time visibility only works if data flows smoothly from patient to clinician without delays or gaps.
“Does it provide predictive insights or risk stratification?”
Predictive analytics can help clinicians identify potential health risks early, allowing for timely intervention. It also helps allocate resources more effectively by identifying high-risk patients.
“Who owns the data, and how easily can it be shared or exported for reporting purposes?”
Make sure you control your data and can use it as needed.
About Security and Compliance
“How do you ensure HIPAA and regulatory compliance?”
Generic answers aren’t acceptable. Ask for specific security protocols, compliance certifications, and audit results.
“What security certifications or audits back this up?”
Independent validation matters more than vendor promises. Ask about security certifications such as SOC 2, ISO 27001, or other third-party audits that verify the vendor’s security practices.
About Scalability
“How well does the system scale for large populations?”
The right vendor should offer services that grow with your practice and adapt to changing requirements. Don’t assume scalability—verify it.
“Can it support multiple conditions and devices?”
You don’t want to manage five different monitoring systems for five different conditions. Ask about the system’s flexibility.
About Finances
“What is the total cost of ownership?”
Include everything: hardware, software, training, support, integration, and maintenance over 5 years. That’s your real investment.
“How does this solution support reimbursement pathways?”
Understanding how the system supports billing and reimbursement is important, especially if you’re pursuing RPM or other reimbursable monitoring programs. Ask vendors what documentation is provided. The level of billing support varies by vendor, and its importance in your decision process will depend on your specific reimbursement model.
About Track Record
“What results have you delivered for similar organizations?”
Size and setting matter. A system that works for a 50-bed rural hospital might not scale for a 500-bed medical center.
“What’s on your product roadmap for the next 2-3 years?”
You’re making a long-term investment. Make sure the vendor’s vision aligns with where your organization and healthcare are heading.
“Can you provide references from similar facilities?”
Talk to real users. Ask them what the vendor didn’t mention during the sales process. That’s where you learn the most.
Beyond the Technology
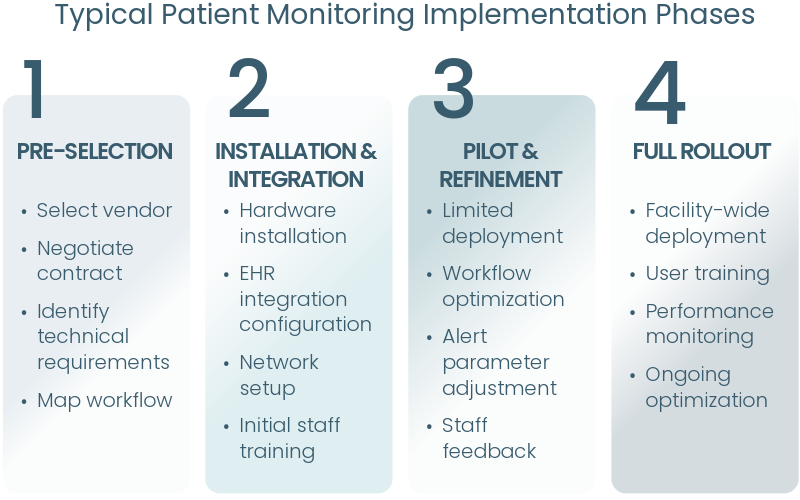
The Implementation Reality Check
Implementation timelines often go beyond the vendor’s original target date. Why? Staff training can take longer than anticipated; data integration may have hiccups; hardware and network configuration don’t always go to plan; and change management can’t be rushed.
Build in buffer time. Identify who on your team will own the project. Define success metrics before you start, not after. And remember, healthcare vendor management involves registration, credentialing, compliance monitoring, and ongoing communication—it’s a continuous relationship, not a one-time transaction.
Patient monitoring system implementation timeline showing four phases over 12 months from planning through full deployment and optimization
Think About Workflow First
The best monitoring system won’t fix broken workflows or unclear protocols.
Before you buy:
- Map your current patient monitoring workflows.
- Identify pain points the technology should address.
- Define what success looks like with specific metrics.
- Plan for the change management required.
Technology should support good workflows, not create workarounds for bad ones.
Look Ahead
Many remote patient monitoring systems measure vital signs at set intervals. But continuous healthcare monitoring is expanding across care settings—in hospitals, post-acute facilities, and home settings where early detection of gradual decline matters most.
Consider where patient monitoring is heading. AI-powered analytics are increasingly common. Interoperability requirements keep tightening. Make sure your chosen system won’t be obsolete before you finish paying for it.
The Bottom Line
Choosing a patient monitoring solution doesn’t have to be overwhelming.
Start with your goals. What outcomes are you trying to improve? Then evaluate vendors against the capabilities and questions outlined here.
Don’t rush it. The challenge of narrowing your options down to a manageable number of vendors is real—but it’s a critical step. Take time for thorough demonstrations. Check references carefully. Test-drive the system with real workflows and real clinicians.
The right monitoring solution becomes an invisible part of care delivery. It helps your team catch problems early, surfaces insights automatically, and makes clinicians more effective without making them work harder.
That’s what you’re looking for. Now you know how to find it.
Have questions about choosing the right patient monitoring system for your facilities? Contact us to discuss your specific needs and see how Neteera’s continuous contactless monitoring technology can support your clinical goals. Let’s start a conversation.


